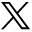The best laid schemes of mice and men, Often go awry
—Robert Burns (To a Mouse, 1785)
To follow on from the excellent articles by Drs. Francisco Jimenez and Jerry Cooley in the last issue of the Forum, here is some more on the subject of hair biology. So why the title from the famous Scottish poet, Robbie Burns? Several years ago, we were enthralled by the prospect of cell therapy—aka “cloning”—as being the ultimate answer to the biggest problem hair transplant surgeons face: donor limitations. We can talk endlessly about the safe donor area, but how can we get beyond this issue? At the moment, we can’t. The big breakthrough came from the pre-clinical mouse models that showed lots of hair growing following injecting dermal papillae cells expanded in culture (Figure 1).
Human hairs growing on a mouse at 5 months.
The concept of cell therapy is that small numbers of hair follicles are harvested from the donor region; separated dermal papilla (DP) cells are then cultured in the lab and then transferred back to the patient’s balding areas.1 These hair forming cells would either organize into new hair follicles, or stimulate the transformation of a vellus hair into a terminal hair. Early studies on these concepts failed because the cells lost their ability to induce hair follicles to grow after they went through several passages of cell cycling. Not until the work with improved culture medium could it be demonstrated that long-term culture was possible whilst still maintaining the ability to grow hair.2 Following on from this work, animal experiments have shown that isolated follicular dermal papilla, cultured dermal papilla, dermal connective tissue sheath cells and bulge epidermal stem cells all can regenerate hair follicles.3-9
So getting back to the poem, unfortunately mice models did not equate to human models. If you recall from the lectures during the Intercytex trials back in 2006-2009, this nice hairy result seen in the pre-clinical mouse models did not happen in the human trials. These trials used a single cell system of dermal papillae cells cultured in keratinocyte cultured medium that, unlike the mouse models, did not grow lots of hair.10 In fact the results that were obtained were probably only slightly better than could be obtained from wound healing response studies alone.11
So, if we are not mice, how do we get past the problem of growing hair in men? Well one answer comes from ground breaking research from Angela Christiano’s lab where they showed that, unlike the mouse model, culture of human DP cells demonstrated a decrease in the genetic function of the aggregates.12 They found that once the DP cells were moved from their natural 3D configuration to growth in culture in a 2D environment that rapid changes occurred in molecular signalling resulting in a loss of ability to form hair follicles. However, when they grew cells as 3D spheroids, partial restoration of induction occurred. Interestingly, in their experiments, spontaneous self-aggregation of DP cells did not occur with human cells injected into the skin in the way that it does with mouse DP. This suggests that previous attempts at hair regeneration in human trials were doomed to fail. The next part of the experiments involved culturing DP cells in hanging drop cultures to mimic cell condensates. These 3D spheroids when injected into human skin partially formed hair follicles in five out of seven cases. The hairs were small, did not contain sebaceous glands, and often didn’t go through the skin surface. On the other hand, control experiments using whole dermal papillae did produce sebaceous glands and normal hair architecture.
Another interesting avenue of research was outlined in Dr. Valerie Horsley’s hair biology lecture on adipose tissue that was presented at the 2015 Annual Scientific Meeting in Chicago. Adipose tissue comprises mature adipocytes and stromal vascular cells, including adipocyte precursor cells (preadipocytes). Preadipocytes have the ability to differentiate into adipocytes whereas adipocyte stromal cells (ASCs) can also differentiate into additional cell types such as osteoblasts and chondrocytes. Dr. Horsley discussed how the hair follicle growth cycle is associated with variability of adipose tissue where the thickness of the intradermal adipocyte layer in the active anagen phase increases significantly compared with the thickness of that in the resting phase of the hair cycle.13 The adipose lineage cells have been reported as regulating HF stem cell activity with the numbers of precursor cells reaching a peak during anagen and a low during catagen.14 However, mature adipocytes appear to exert a negative effect as shown in experiments by Misago et al where proliferation of perifollicular fibroblasts was inhibited by fat cells.15 Other researchers demonstrated that mature intradermal fat cells expressed BMP2 messenger RNA (mRNA), which is an inhibitory signal for bulge cell activity.16 Collectively, these research projects have demonstrated that the stromal vascular layer in fat shows positive effects on DP cells hair-inducing ability; however, despite this recent progress in the lab, there are still many unknowns in understanding of basic dermal papilla and adipocyte cell biology and their interactions.
In recent years, some doctors have started to offer patients stem cell therapy for adult human hair-follicle neogenesis, and so far the laboratory research supports these attempts at treatment in the clinic. However, hair follicle cell therapy continues to be an attractive topic in regenerative medicine, partly due to the ease of obtaining hair and skin cells. Because there is also now a good foundation of hair follicle biology research, and with the continued clinical interest, there is no doubt that someone will finally find the missing pieces to the puzzle.
- Copyright © 2015 by The International Society of Hair Restoration Surgery